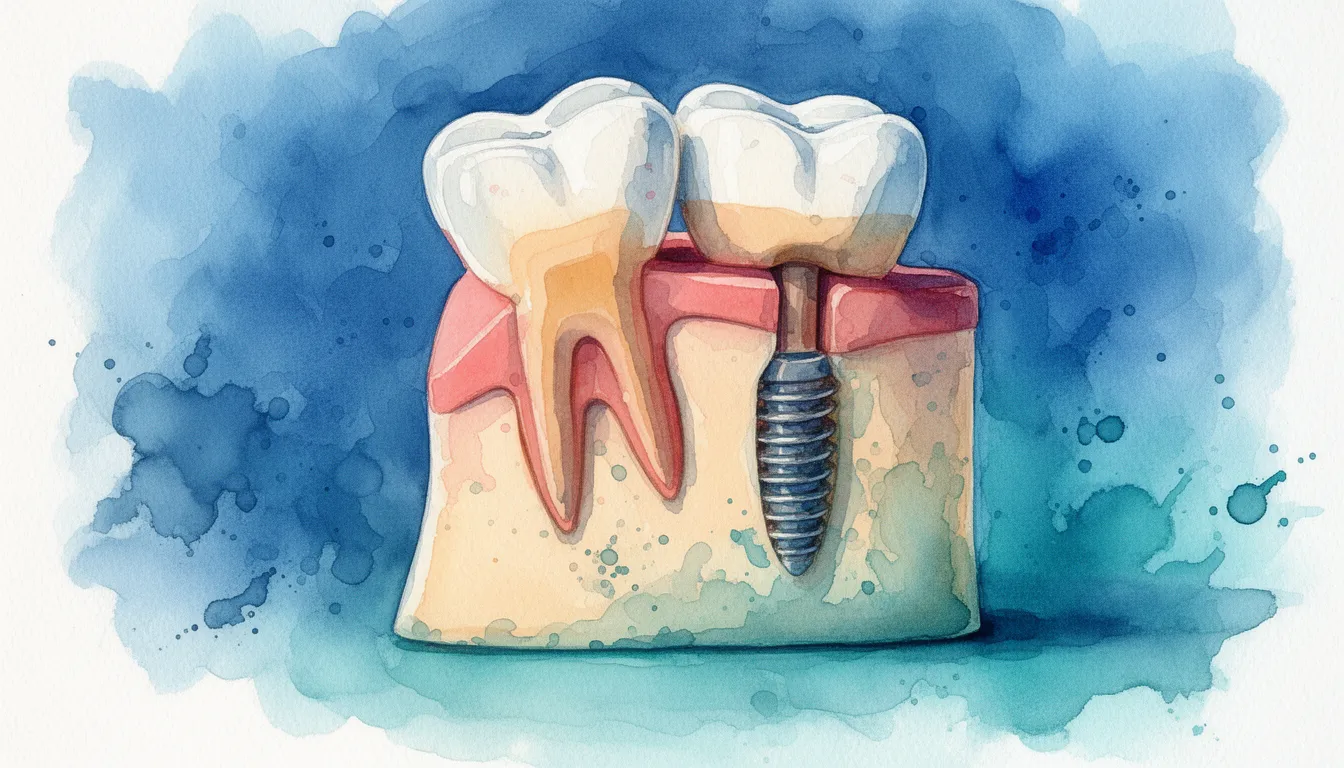
What Is Bone Loss in the Jaw?
Bone loss in the jaw is the gradual reduction in the volume and density of the alveolar bone, the ridge of bone that holds your teeth in place. This process is called alveolar ridge resorption.
Your jawbone stays healthy partly because of the mechanical stimulation it receives every time you chew. When a tooth is lost or removed, that stimulation stops. The body begins to reabsorb the bone in that area because it no longer senses a functional need for it. This same process can happen when advanced gum disease destroys the bone that surrounds tooth roots.
Jaw bone loss is extremely common. Research shows that peri-implantitis, a condition involving bone loss around dental implants, affects a significant portion of implant patients. A Swedish population study of over 4,700 implant patients found that 14.5% had moderate to severe peri-implantitis at a nine-year follow-up, while up to 45% showed some sign of the condition when mild forms were included. [5] This highlights how bone loss remains a concern even after teeth have been replaced with implants and underscores the need for ongoing professional monitoring.
Understanding the causes and warning signs of bone loss can help you take steps to slow or reverse the process. The earlier it is caught, the more treatment options are typically available.
Causes and Risk Factors for Jaw Bone Loss
Jaw bone loss is typically caused by tooth loss, gum disease, or conditions that reduce stimulation to the bone.
Tooth Loss and Extraction
The most direct cause of alveolar bone loss is tooth extraction or traumatic tooth loss. Once a tooth is gone, the surrounding bone no longer receives the forces of chewing. Without that stimulation, the bone begins to shrink. Most studies report that the majority of bone resorption occurs within the first six to twelve months after extraction.
The extent of early bone loss can be substantial. A systematic review by Tan et al. (2012) found that alveolar ridge width decreased by 29% to 63% within the first six months after extraction. [10] A study by Schropp et al. (2003) involving 46 extraction sites reported a mean reduction in ridge width of about 50% after twelve months. [11] These findings illustrate why many providers recommend socket preservation grafting at the time of extraction to reduce this early bone loss.
A systematic review of implants placed into fresh extraction sockets confirmed that early bone remodeling is a predictable event after tooth removal. [7] Over time, the ridge can narrow and shorten, changing the shape of your jaw and face.
Periodontal (Gum) Disease
Periodontitis is a chronic bacterial infection of the gum tissue and bone around teeth. As the infection progresses, it destroys the attachment fibers and bone that hold teeth in place. According to the American Academy of Periodontology, periodontitis is a leading cause of tooth loss in adults. [8]
The bone loss caused by gum disease tends to happen unevenly. Some teeth may lose significant bone support while neighboring teeth remain stable. This irregular pattern can complicate treatment planning for implants or other restorations.
Long-Term Denture Wear
Traditional dentures rest on top of the gum and bone ridge. They do not transmit chewing forces into the bone the way natural tooth roots or implants do. Over years of denture wear, the underlying ridge continues to resorb. This is why dentures often become loose over time and need to be relined or remade.
A study of patients aged 75 and older who wore implant-retained overdentures in the lower jaw found that peri-implant health and bone levels varied. Even with implant support, ongoing monitoring was needed to manage bone changes. [6]
Other Risk Factors
Several systemic and lifestyle factors can accelerate bone loss in the jaw. These include smoking, uncontrolled diabetes, osteoporosis, certain medications such as long-term corticosteroids, and radiation therapy to the head and neck region.
A systematic review and meta-analysis examining advanced age and systemic medical conditions found that while dental implants can still succeed in older or medically compromised patients, certain conditions may influence bone stability and implant survival rates. [4]
- Smoking reduces blood flow to bone and gum tissue, slowing healing and accelerating bone breakdown.
- Diabetes (when poorly controlled) impairs the body's inflammatory response and can worsen periodontal bone loss.
- Osteoporosis affects bone density throughout the body and may contribute to faster jaw resorption.
- Medications such as bisphosphonates, while treating osteoporosis, can in rare cases cause jawbone complications.
- Radiation therapy to the jaw area can damage bone cells and reduce the bone's ability to heal.
Symptoms and Diagnosis of Jaw Bone Loss
Jaw bone loss often develops silently, with no pain in the early stages.
What Patients Typically Notice
In the early stages, you may not feel anything at all. Bone loss inside the jaw is not usually painful until it becomes advanced. The first signs patients tend to notice are changes in how their teeth fit together or how their dentures feel.
As bone loss progresses, symptoms may become more obvious. Teeth may start to feel loose. Gums may recede, making teeth look longer. Dentures may slip or cause sore spots. In advanced cases, the lower face can appear shorter or the chin may seem to protrude more. These facial changes happen because the bone that supports the lower third of the face has shrunk.
- Teeth that feel loose or shift position
- Gum recession (gums pulling away from teeth)
- Dentures that no longer fit well
- Changes in facial appearance, especially around the mouth and chin
- Difficulty chewing or bite changes
- Gaps developing between teeth that were previously close together
How Bone Loss Is Diagnosed
Dentists and periodontists diagnose bone loss using a combination of clinical examination and imaging. During a periodontal exam, the provider uses a small probe to measure the depth of pockets between your gums and teeth. Deeper pockets often indicate that bone has been lost around that tooth.
Dental X-rays, especially panoramic X-rays or periapical films, show the level of bone around each tooth. For implant planning, a cone-beam computed tomography (CBCT) scan provides a three-dimensional view of bone width, height, and density. This detailed image helps the specialist determine whether enough bone exists for implant placement or whether grafting will be needed. The American Dental Association recommends regular dental visits as a key part of catching problems like bone loss early. [9]
When to Seek Care
You should contact a dentist or periodontist if you notice loose teeth, bleeding gums that persist for more than two weeks, receding gums, or changes in your bite. If you have been wearing dentures for several years and they no longer fit well, that is also a sign that bone loss may be progressing. Early diagnosis gives you the widest range of treatment options.
Treatment Options for Jaw Bone Loss
Treatment depends on the severity of bone loss and your long-term goals for replacing missing teeth.
Bone Grafting
Bone grafting is a surgical procedure that adds bone material to areas of the jaw where bone has been lost. The graft material can come from your own body (autograft), a human donor (allograft), an animal source (xenograft), or a synthetic material (alloplast). The graft acts as a scaffold that encourages your body to grow new bone in the area.
Bone grafts are commonly performed at the time of tooth extraction to preserve the socket for a future implant. Given that research shows the ridge can lose 30% to 60% of its width in the first six to twelve months after extraction, socket preservation grafting plays an important role in maintaining enough bone for later implant placement. [10] [11] Grafts are also used months or years after extraction when the ridge has already resorbed. Healing typically takes three to six months before the grafted area is ready for implant placement.
Ridge Augmentation
Ridge augmentation is a specific type of bone grafting aimed at rebuilding the height or width of the alveolar ridge. When the ridge has become too narrow or too short to support an implant, the periodontist or oral surgeon rebuilds it using graft material, often combined with a membrane that guides bone growth. This procedure is sometimes called guided bone regeneration (GBR).
Ridge augmentation can add several millimeters of bone width and height in many cases. Results vary depending on the extent of the original defect, the patient's healing ability, and the graft material used.
Sinus Lift (Sinus Floor Elevation)
A sinus lift is a bone grafting procedure specific to the upper jaw. The maxillary sinuses sit just above the roots of the upper back teeth. When those teeth are lost and bone resorbs, the sinus floor drops, leaving too little bone height for implant placement.
During a sinus lift, the surgeon gently lifts the sinus membrane upward and places bone graft material beneath it. This creates enough bone height to anchor an implant. Healing typically takes four to nine months before implants can be placed.
Dental Implants
Dental implants are titanium posts surgically placed into the jawbone to replace missing tooth roots. Once integrated with the bone (a process called osseointegration), they support crowns, bridges, or dentures. Implants are the only tooth replacement that transmits chewing forces directly into the bone, which helps preserve bone levels.
A systematic review of immediately placed implants found survival rates typically above 95% at one year or more. [7] However, bone loss can still occur around implants. A retrospective study found that early implant bone loss during the preprosthetic phase (the healing period before the final crown is placed) varied based on factors such as implant position and loading protocol. [2]
Even after successful placement, ongoing vigilance is important. A Swedish study of over 4,700 patients found that 14.5% developed moderate to severe peri-implantitis within nine years, with up to 45% showing at least mild signs of the condition. [5] This means that while implants are highly successful overall, regular professional monitoring remains essential to catch bone-related changes early.
For patients with significant bone loss who want to avoid extensive grafting, some implant systems use angled placement or shorter implants to work with the available bone. A systematic review of implant-supported fixed prostheses with cantilever extensions found that these designs can be effective, though they require careful planning. [1] Complications in implant dentistry, including bone-related issues, tend to cluster in certain patients, suggesting that individual risk factors play a major role. [3]
Treating the Underlying Gum Disease
When bone loss is caused by periodontal disease, treating the infection is the first priority. This typically starts with scaling and root planing (a deep cleaning that removes bacteria and tartar from below the gumline). In more advanced cases, surgical procedures such as flap surgery or regenerative procedures may be needed to clean deep pockets and encourage bone regrowth.
The American Academy of Periodontology notes that early treatment of gum disease is critical because bone lost to periodontitis does not fully regrow on its own. [8] Ongoing maintenance visits, usually every three to four months, are essential to prevent recurrence.
Recovery and Aftercare
Recovery time varies by procedure, but most bone grafting and implant surgeries involve several months of healing.
Typical Recovery Timeline
After a bone graft, expect mild to moderate swelling and discomfort for the first few days. Most patients manage this with over-the-counter pain relievers or a short course of prescribed medication. Soft foods are recommended for the first one to two weeks.
The graft itself takes time to mature. Most providers wait three to six months before placing an implant into a grafted site. Sinus lifts may require four to nine months of healing. Your specialist will use X-rays or a CBCT scan to confirm that enough new bone has formed before proceeding.
- Days 1 to 7: Swelling peaks around day two or three, then gradually decreases.
- Weeks 2 to 4: Soft tissue heals over the graft site. Stitches are removed if non-dissolving sutures were used.
- Months 3 to 6: Bone graft matures and integrates. Follow-up imaging confirms readiness for the next step.
- Months 4 to 9 (sinus lift): Longer healing window due to proximity to the sinus cavity.
Follow-Up Care and Maintenance
After implant placement, long-term follow-up is essential. Peri-implantitis (infection and bone loss around an implant) can develop if oral hygiene is inadequate or if risk factors like smoking are present. The Swedish population study found that 14.5% of implant patients had moderate to severe peri-implantitis at nine years, with up to 45% showing at least mild signs when all forms were counted, underscoring the need for regular professional monitoring. [5]
Your provider will typically schedule follow-up appointments at specific intervals after surgery, then transition you to maintenance visits every three to six months. These visits include probing around implants, checking for signs of inflammation, and taking periodic X-rays to monitor bone levels.
Cost Factors for Bone Loss Treatment
The cost of treating jaw bone loss depends on the type and extent of the procedure needed. Costs vary by location, provider, and case complexity.
A simple socket preservation bone graft at the time of extraction may range from $300 to $800 per site. Larger block grafts or ridge augmentation procedures typically range from $1,500 to $3,500. Sinus lifts generally cost between $1,500 and $5,000 per side, depending on whether a lateral or crestal approach is used.
Dental implant costs vary widely. A single implant with the abutment (connector) and crown typically ranges from $3,000 to $6,000. If bone grafting is also needed, the total cost per tooth can reach $8,000 to $10,000 or more. Full-arch implant-supported restorations are significantly more expensive, often ranging from $20,000 to $45,000 per arch.
Dental insurance may cover a portion of bone grafting or periodontal surgery if it is deemed medically necessary. Coverage for implants varies greatly by plan. Many dental offices offer payment plans or work with third-party financing companies. Ask your provider's office about your specific coverage before treatment begins.
When to See a Specialist
A periodontist is the specialist most trained to diagnose and treat bone loss around teeth and implants.
General dentists can identify bone loss on X-rays and treat mild gum disease. However, moderate to severe bone loss, bone grafting procedures, sinus lifts, ridge augmentation, and complex implant cases typically require a periodontist or oral surgeon. Periodontists complete an additional three years of training beyond dental school, focused specifically on the supporting structures of teeth: the gums, bone, and connective tissue.
If your general dentist has told you that you have significant bone loss, or that you need a bone graft before an implant, a referral to a periodontist is a reasonable next step. You can learn more about what periodontists do and find a provider near you on the periodontics page.
For patients with systemic conditions such as uncontrolled diabetes or osteoporosis, a specialist can work with your medical team to manage the added risks. A systematic review confirmed that while advanced age and systemic conditions can influence implant outcomes, careful patient selection and treatment planning help achieve favorable results in many cases. [4]
Find a Periodontist Near You
If you have been told you have bone loss in your jaw, or if you are experiencing loose teeth, receding gums, or ill-fitting dentures, a periodontist can evaluate your bone levels and discuss your treatment options. Use the My Specialty Dentist directory to find a qualified periodontist in your area and take the next step toward protecting your jaw health. Visit the periodontics page to get started.
Search Periodontists in Your Area